
Hearing Aids
Penn Medicine Becker ENT & Allergy provides a specialized and comprehensive team of ENT Doctors dedicated to improving the quality of life for those with hearing loss. With the help of a qualified doctor, individuals can access a variety of state-of-the-art hearing aids that can help them restore their hearing and take part in activities they may have previously been unable to enjoy. Through the use of advanced technology, Penn Medicine Becker ENT & Allergy strives to provide an individualized solution for each patient’s unique needs.
Our audiology team works in partnership with our New Jersey and Philadelphia ENT specialists to provide individualized treatment plans and ensure that all of our patients’ ear-related issues are properly addressed.
Hearing loss, recurrent and chronic ear infections, ear wax buildup, dizziness, eardrum perforations, ear fullness, Eustachian tube dysfunction, and tinnitus (ringing in the ears) are just some of the ear conditions treated by physicians at Penn Medicine Becker ENT & Allergy.
Hearing Healthcare Services

Hearing Aids Service
Modern technology provided with specialized treatment plans

Hearing Loss Prevention
Prevention of some forms of hearing loss and tinnitus for all ages

Pediatrics
Prevention and treatment of hearing loss and speech & language delays in children
What Is a Hearing Aid?
A hearing aid is a small electronic device that amplifies sound. It is composed of four basic parts – a microphone that picks up sound, an amplifier that increases the volume of the sound, a speaker that plays the amplified sound, and a battery that powers the device. Sound waves are picked up by the microphone, which then converts them into electrical signals that are sent to the amplifier. The amplifier increases the volume of the sound, which is then played back through the speaker.
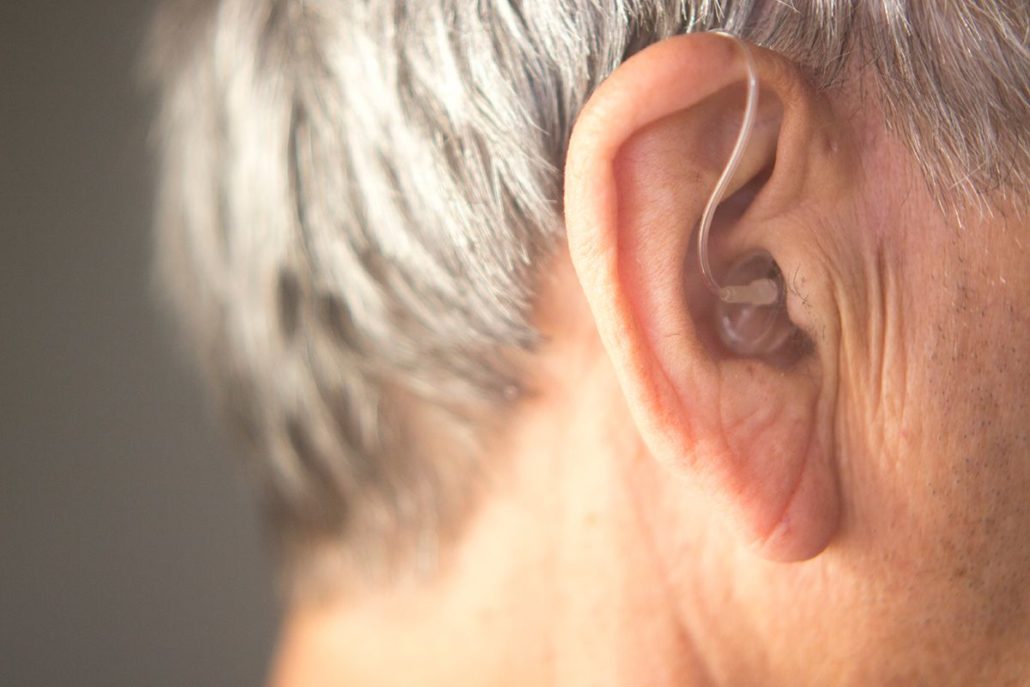
Recognizing the Onset of Hearing Issues
As we age, our hearing abilities can gradually diminish. Pay attention to symptoms such as gradual hearing loss, tinnitus, misophonia, and hyperacusis, which may indicate the need for a hearing test. Seeking help early is crucial because delaying treatment can lead to permanent damage. The common causes of hearing loss include age-related hearing loss and noise-induced hearing loss. To prevent it, wear ear protection in loud environments and be mindful of your noise consumption. Don’t hesitate to get a hearing test if you’re experiencing any of these symptoms.
Benefits of Wearing Hearing Aids
When it comes to managing hearing loss, hearing aids are a popular and effective solution. These medical devices offer a range of benefits for those experiencing difficulties with ear hearing. As previously mentioned, properly amplified sound and improved speech comprehension are just a few of the benefits that hearing aids can provide. But there are many other hearing benefits as well. For example, wearing hearing aids can enhance an individual’s overall quality of life by reducing feelings of isolation and promoting a greater sense of independence and confidence.
There are many different types of hearing aids available, each with its own unique features and capabilities. From behind-the-ear models to discreet, virtually invisible in-the-canal options, there is a wide range of choices to fit individual needs and preferences. It’s important to work with a hearing care specialist to determine the best type of hearing aid for each individual, based on their specific hearing loss and lifestyle.
Of course, one factor that many people consider when choosing a hearing aid is the cost. While aid prices can vary depending on the type and model of the hearing aid, it’s also worth considering the long-term hearing benefits that may be gained by investing in this type of medical device. Ultimately, the most important consideration is finding a solution that works best for the individual, and that will help improve their overall ear hearing and quality of life.
Types of Hearing Aids
There are different types of hearing aids to suit individual hearing needs. These devices come in different shapes, sizes, and styles, ranging from behind-the-ear (BTE) hearing aids, receiver-in-canal (RIC) hearing aids, in-the-ear (ITE) hearing aids, in-the-canal (ITC) hearing aids, and completely-in-canal (CIC) hearing aids. The selection of an appropriate hearing aid for a patient is contingent upon several factors, including the extent of hearing loss, lifestyle, individual preferences, and budgetary considerations.
In-the-Ear (ITE) Hearing Aid
In-the-Canal (ITC) Hearing Aid
Completely-in-Canal Hearing Aid
Digital Hearing Aids
An In the Ear (ITE) Hearing Aid sits in the ear canal and is designed to amplify sound for those with mild to severe hearing loss. ITE hearing aids come in different sizes and models with various features, such as rechargeable batteries, directional microphones, and digital noise reduction. Many brands, including Audien, Widex, Starkey, and Oticon, offer ITE hearing devices. ITE hearing aids are appropriate for many types of hearing loss and can improve the quality of life for those experiencing hearing difficulties.
The In the Canal (ITC) hearing aid sits deep within the ear canal and is larger than the Completely in Canal aid. Its small size provides discretion and easy handling. Directional microphones improve hearing in noisy environments. Battery life can last up to a week, and a one-year warranty is standard. However, susceptibility to moisture and earwax buildup can affect performance. Suitable for those with mild to moderate hearing loss, the ITC offers benefits like a discreet appearance and improved hearing in noisy situations. Its limitations include susceptibility to moisture and earwax buildup.
Completely in the Canal Hearing Aids are custom-made to fit deep within the ear canal, rendering them almost invisible. The advantages of this model include cosmetic appeal and reduced wind noise. However, this style may amplify noises such as chewing and breathing (occlusion effect) and is not suitable for those with profound hearing loss. This model’s deep-seated placement makes it an excellent choice for those who frequently use telephones without feedback, particularly those with mild to moderate hearing loss.
Digital hearing aids process sound differently from analog ones. They convert sound waves into a numerical code which can be manipulated to enhance specific frequencies that the wearer struggles to hear. This means that they have superior speech separation and background noise reduction features, making conversations easier to follow. They also have multiple programs, allowing wearers to adjust settings in different listening environments. Digital technology can cater to specific hearing loss requirements, covering a wide average price cost range with various advantages over analog alternatives.
Candidates for Hearing Aids
Hearing loss can be objectively measured through hearing exams. This vital assessment is typically conducted by an audiologist as part of a comprehensive hearing evaluation. Utilizing specialized equipment, the audiologist can accurately determine the presence and extent of hearing loss in each ear, as well as identify any specific areas of the hearing system that may be impaired. This valuable knowledge serves as a foundation for directing appropriate treatment options, such as recommending an optimal hearing aid or listening device.
It’s important to note that many individuals experience hearing loss in both ears. In such cases, the best outcomes are often achieved with the use of two hearing aids. Recognizing that each patient is unique, our dedicated team of audiologists collaborates to assess and determine the most suitable hearing instruments based on individual listening needs, budgetary considerations, and personal abilities. By taking these factors into account, we strive to provide the best possible solutions for our patients’ hearing health.
The Cost of Hearing Aids
Hearing aid prices can vary widely due to factors such as technology level, design, and features. Prescription hearing aids typically cost more than over-the-counter options since they are customized to the wearer’s specific hearing needs. While over-the-counter hearing aids may be cheaper, they lack the advanced features that prescription devices offer. Purchasing from a hearing professional offers benefits such as expertise, fitting, follow-up care, and the ability to use financing options, private health insurance, Medicaid, flexible spending accounts, and veterans’ benefits to cover the cost.
Choosing the Right Hearing Aid
Hearing aids are sophisticated devices that come in many styles and sizes. There are different types of devices available such as behind-the-ear (BTE), in-the-ear (ITE), in-the-canal (ITC) and completely-in-canal (CIC). The choice of hearing aid largely depends on the degree of hearing loss, medical conditions, budget and personal preferences of the user. A hearing care professional can help identify the best hearing aid type and features that suit individual needs.
Different Styles, Technologies, and Features Available
Hearing aids come in various styles, from behind-the-ear to completely-in-canal, each designed to meet different needs. Rechargeable batteries are a popular feature that eliminates the need to replace batteries frequently. Digital noise reduction technology can help reduce unwanted background noise for a better listening experience. Other features include directional microphones, Bluetooth connectivity, and self-fitting options. It’s essential to consult a hearing care professional to find a device with the right style, technology, and feature combination for individual needs.

Maintenance and Care of Hearing Aids
Proper maintenance of hearing aids is crucial to keep them functioning properly. Check the batteries regularly and have spares on hand. Clean the hearing aid as per the audiologist’s instructions using specialized tools for hearing aid care. Store them properly in a dry place. Listening checks can help you recognize when a hearing aid needs maintenance. A hearing care specialist can provide additional tips for maintaining your hearing aids.
Many patients have hearing loss in both ears. In these situations, optimal results are usually obtained with 2 hearing aids. Every patient is different. Our audiologists work as a team to determine the best possible hearing instruments for each patient’s listening needs, budget, and abilities.

Pick one of our convenient locations
for your Hearing aid Treatment